Have you got a positive in your home pregnancy test? There are few moments in life that provoke such a strong sense of emotion. Maybe you have been trying for months, or maybe this came as more of a surprise – no matter what, it is a life-changing moment.
Your next step should be to let your OBGYN know. While many providers don’t recommend the first routine pregnancy ultrasound appointment until 9-10 weeks gestation, some offer an earlier ultrasound around 6-8 weeks, often called a viability check. Your provider may especially want to do this depending on your history or certain risk factors, or if you have had repeated pregnancy loss. You are also a good candidate for a viability check if you are unsure of the date of your last menstrual period, which is typically what is used to determine due date and predict how far along a pregnancy is. For this reason, this ultrasound is sometimes called a ‘dating scan’.
Wondering How to Calculate How Far Along You Are?
Pregnancy is 40 weeks long, and that clock starts on the first day of your last menstrual period, which is usually about two weeks prior to ovulation and conception. You read that right – that’s two bonus weeks of pregnancy in the bag by the time you actually conceive!
Your Baby at 7 weeks
At 7 weeks, your baby is still considered an embryo (and will be until 10 weeks). He or she is tiny – about a quarter to a half an inch long and less than a quarter ounce in weight. Right now, your baby is the size of a blueberry or a chickpea.
Your baby’s brain is developing rapidly as cells multiply at an exponential rate. For this reason, the head is growing more quickly than the rest of the body. Little limbs are also starting to form; right now, they are made up of cartilage that will eventually develop into bone.
The Viability Check Ultrasound Scan
To get the best look at the fetus, this ultrasound scan will be done transvaginally (versus abdominally – which is usually how ultrasounds in the second trimester and third trimester are done). Don’t worry, transvaginal ultrasounds don’t need to be done with a full bladder like you may have heard, so go ahead and use the bathroom before your appointment! The transvaginal ultrasound will be done by inserting a long, thin wand, or ‘transducer,’ a few inches into your vaginal canal until it reaches your cervix. While it may be slightly uncomfortable, it should not be painful.
During the scan, one of the first things your provider will do is ensure the embryo has implanted inside of your uterus rather than somewhere else, like in the fallopian tube. A pregnancy in which the fetus grows outsides the uterus is called an ectopic pregnancy. Unfortunately, ectopic pregnancies are not viable and can be dangerous for mom if left undetected.
The next thing your provider will look for is cardiac activity, or a heartbeat. There should be a fetal pole, which can be detected as early as 6 weeks gestation. The fetal pole can be seen attached to the yolk sac, and is the first sign that an embryo is forming. An expected fetal heart rate at this stage is 90-110 beats per minute. As the embryo develops into a fetus, this rate will actually increase.
Your provider should also be able to see a yolk sac, which is a roundish pouch that serves as the baby’s source of nutrients and cells until the placenta eventually takes over. By weeks 14-20, the yolk sac will gradually get smaller and disappear.
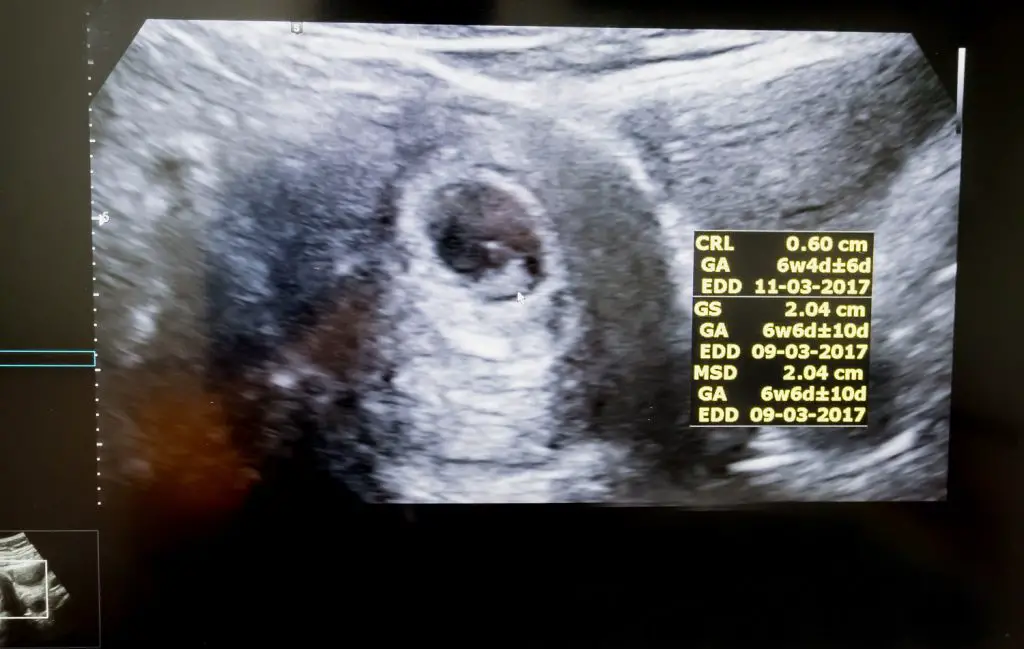
Unfortunately, you won’t be able to see much of what you’d expect a baby to look like at this ultrasound. The embryo is still very small, and his or her shape has yet to take form. Still, that little blob is YOUR little blob, and its heartbeat will be music to your ears! When you come back for another ultrasound in just a few short weeks, you might be shocked by the growth and development of your baby – no wonder you’ve been feeling so tired!
Based on measurements, your provider should be able to confirm your gestational age and due date. If measurements are off from the calculations using your last period, he or she may ask you to come back in a week or two to perform some additional measurements.
What else can you expect from this visit?
Your doctor may want to order a blood test called a Quantitative Beta Human Chorionic Gonadotropin test – or Beta HCG test. This test measures the levels of the HCG hormone produced in the body during pregnancy. This test is usually done twice, about 48 hours apart (so, if you have the first on a Tuesday at 2pm, you’ll have another on Thursday at 2pm). HCG levels rise rapidly during the first trimester. Once your doctor gets the second result back, he or she will be able to see whether your levels are rising appropriately. If they are not, it is an indication that the pregnancy is not viable and will likely result in miscarriage.
If you’re feeling unpleasant early symptoms of pregnancy – fatigue, nausea, swollen or tender breasts, etc. – this visit is a good opportunity to chat with your provider about safe treatment. Be sure you’re staying hydrated, getting lots of rest, and leaning on your partner, family, and friends for support. Your provider will offer helpful tips about over the counter medications or at home remedies you can try, and he or she may even prescribe an anti-nausea medication if necessary. Be sure to ask any additional questions you have at this visit – a new pregnancy comes with a lot of uncharted territory and, rest assured, it has all been asked before!
When is the Next Ultrasound Scan?
If your pregnancy is viable, your doctor will likely ask you to schedule another routine ultrasound around 10 weeks gestation (read our article on the 10 week ultrasound scan). You can also expect an ultrasound around 18-20 weeks, called the Anatomy Scan, which will entail taking a closer look at your baby’s bones and organs; and another, done in the Third Trimester (at around 36-38 weeks) that provides an estimated weight of your baby, measures the amount of amniotic fluid you have, and checks the baby’s positioning prior to birth.
What if you Find out the Pregnancy is Not Viable?
It is a difficult truth that one in four pregnancies end in miscarriage. Most often, this will happen in the first trimester, or before the 13th week of pregnancy. After week 6, risk drops to 10%, and continues to gradually decrease as the weeks go on. Most miscarriages are caused by chromosomal abnormalities that make future viability impossible. If this happens, whatever you do, try not to blame yourself. The good news is that the likelihood of having a subsequent miscarriage is low. Talk to your provider about when it’s safe for you to start trying again and don’t be afraid to seek the support of a therapist or support group in your area.
Read More of Our Series on Ultrasound Scans
The Viability Check Ultrasound Scan
Routine blood tests during pregnancy: Our guide to the blood tests you’ll be recommended during pregnancy